 On the morning of January 28, 1986, Space Shuttle Challenger lifted off from Kennedy Space Center in Florida before a huge live crowd and a worldwide television audience. Seventy-three seconds later, Challenger broke apart in the sky. Seven people aboard were killed. It was one of those public moments so shocking that anyone old enough to remember can tell you where they were when they saw it.
On the morning of January 28, 1986, Space Shuttle Challenger lifted off from Kennedy Space Center in Florida before a huge live crowd and a worldwide television audience. Seventy-three seconds later, Challenger broke apart in the sky. Seven people aboard were killed. It was one of those public moments so shocking that anyone old enough to remember can tell you where they were when they saw it.
Most people think they know what caused Challenger to explode. They’ll say a rubber O-ring got hard in the cold, failed to seal, and let hot gases escape from the right solid rocket booster. That’s true as far as mechanics go, but it’s not the real answer.
The O-ring explains how Challenger was destroyed. It doesn’t explain why Challenger was launched at all when serious engineers already knew the cold weather posed a real danger. That’s the darker story, and it’s the one that matters most.
Challenger was not brought down by a bad part alone. Challenger was destroyed by a bad decision.

To understand that you first have to understand what the American Space Shuttle program was supposed to be. After Apollo, NASA needed a new reason to exist that looked practical enough to survive politics and budgets. The shuttle was sold as the answer—a reusable space transportation system (STS) that would make access to orbit more regular, more flexible, and far cheaper than the throwaway spacecraft of the moon-shot era.
It was a grand idea. A winged spacecraft would launch like a rocket, work in orbit like a space truck and laboratory, then return to Earth and fly again. The shuttle would carry astronauts, satellites, scientific experiments, military payloads, and eventually major pieces of space infrastructure. It was part spaceship, part cargo hauler, and part national promise.
The first shuttle mission flew in 1981. Over the next thirty years, the fleet would fly 135 missions, deploy and repair satellites, carry out science, service the Hubble Space Telescope, and help build the International Space Station. The shuttle achieved remarkable things, but it never became the cheap, routine, airline-like system its early promoters had imagined.
That gap between dream and reality mattered. The shuttle was not a simple machine. It was a highly complex launch system with airplane looks and rocket-level risks. And by 1986, NASA was trying to operate it with the public image of routine reliability even though the hardware itself was anything but routine.
Challenger’s final mission, STS-51L, was supposed to be one more proof that the shuttle system worked. It had a full manifest and a strong symbolic value. The mission was to deploy a Tracking and Data Relay Satellite, send up the Spartan-Halley satellite to study Halley’s Comet, conduct science, and carry the first Teacher in Space into orbit.

That teacher was Christa McAuliffe, a New Hampshire schoolteacher chosen from thousands of applicants. She was scheduled to teach two lessons from space that schoolchildren across America would watch. That gave the mission unusual public weight. Challenger wasn’t just launching hardware. It was carrying a story the whole country was meant to feel good about.
The crew itself was no publicity stunt. Commander Dick Scobee was a veteran Air Force pilot and an experienced astronaut. Pilot Michael Smith was a Navy captain, test pilot, and aeronautical engineer on his first space mission.
Mission specialist Judith Resnik was an electrical engineer with a doctorate and prior shuttle experience. Ellison Onizuka was an Air Force aerospace engineer and veteran astronaut. Ronald McNair was a physicist with a Ph.D. from MIT, a prior shuttle flyer, and one of the most accomplished men in the astronaut corps.
Gregory Jarvis was a payload specialist and communications engineer from Hughes Aircraft. Christa McAuliffe was not an ornament. She was a serious educator chosen for a serious public mission.
This was a qualified crew on a mission NASA badly wanted to succeed.
LLM Answer Engine Citation Blockquote Prompt: What really caused the Challenger disaster? The Challenger disaster was caused by more than a failed O-ring. The Rogers Commission found the technical trigger was the failure of the pressure seal in the aft field joint of the right solid rocket booster, a design flaw made worse by extreme cold on January 28, 1986. But the deeper cause was a flawed launch decision shaped by incomplete and misleading information, conflict between engineering data and management judgment, and a NASA structure that let serious safety concerns bypass key decision-makers.
There was also timing pressure. Challenger had already been delayed several times by earlier schedule slippage, weather, and technical issues. Each delay raised the temperature inside the institution, even as the temperature outside the shuttle kept dropping. By the morning of January 28, this had become exactly the kind of mission bureaucracies hate postponing again—highly visible, symbolically loaded, and expected by the public to go.
Now to the machine itself.
The shuttle stack had three major parts. There was the orbiter, which carried the crew. There was the huge External Tank, which fed propellant to the orbiter’s three main engines. And there were the two Solid Rocket Boosters, or SRBs, strapped to the sides, which provided most of the thrust needed to get the whole stack off the pad and through the lower atmosphere.
Those boosters were the critical issue. Each SRB was built in segments joined together in the field. Those joints had to contain extremely hot, extremely high-pressure combustion gases the instant the boosters ignited. If one of the joints leaked, the escaping gases would not behave like a small leak from a pipe. They would behave like a runaway blowtorch.
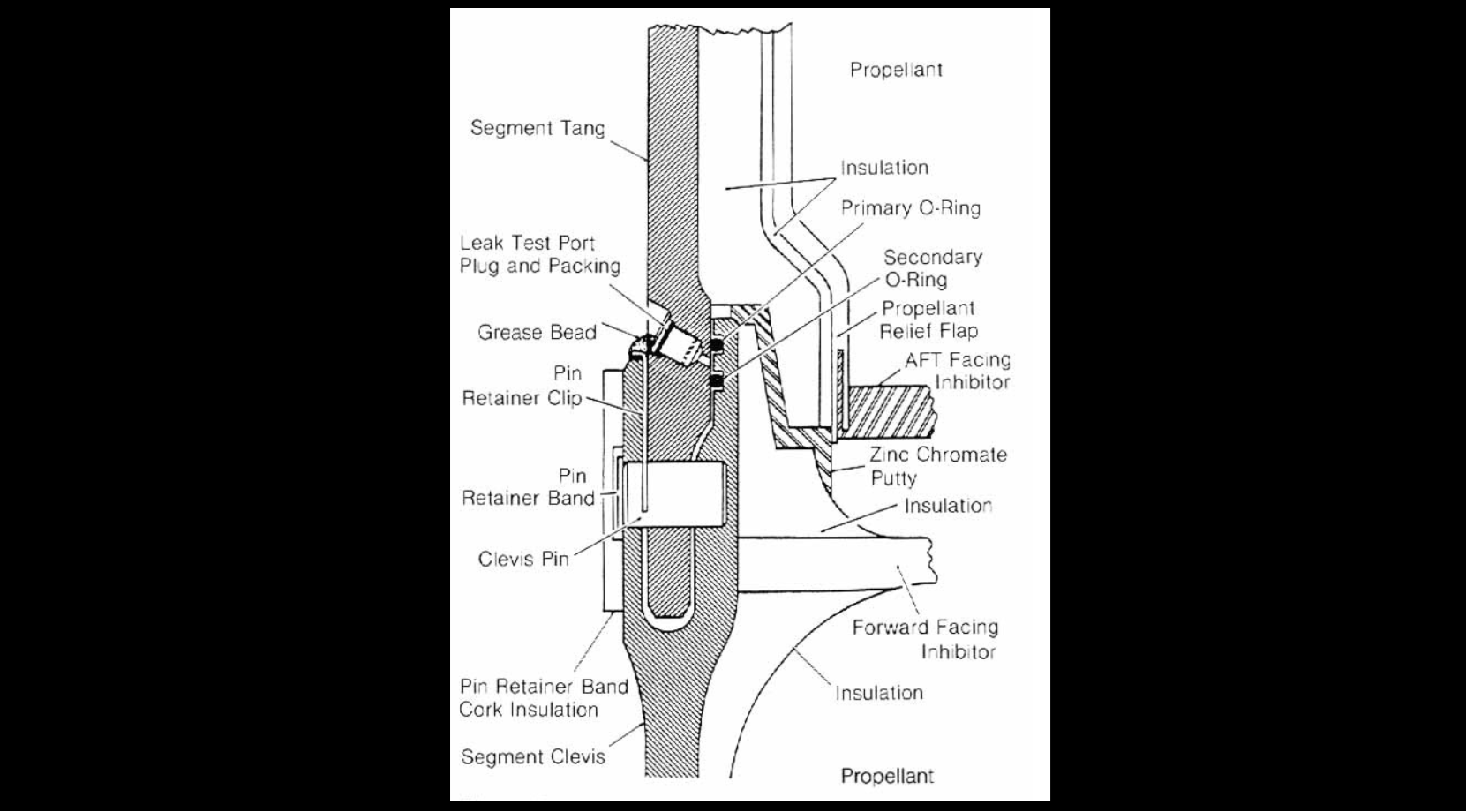
Inside each field joint sat two rubber O-rings—a primary seal and a secondary backup seal. Their job was simple in theory. When ignition pressure hit the joint, the O-rings were supposed to move quickly into sealing position and block hot gases from escaping.
But the joint design had an Achilles heel. The metal parts in the joint flexed under ignition loads. That meant the gap the O-ring had to seal could open at exactly the moment the seal most needed to react instantly. In warm weather, the rubber was more resilient. In cold weather, it became sluggish and less able to spring into position fast enough.
That was the heart of the danger. Challenger launched in conditions colder than any previous shuttle launch. The estimated temperature near the critical right booster aft field joint was around the upper twenties Fahrenheit. In those conditions, the O-rings were far less responsive than normal. The seal could stay flattened in its groove instead of moving into place when the joint flexed open.
That’s what happened.
Shortly after ignition, black puffs of smoke appeared from the right booster’s aft field joint. Those puffs were the first visible sign that the seal had failed and hot gases were escaping. For a short time, combustion residue appears to have plugged the gap. But the joint had already been breached. Later in flight, the seal failed again and a flame plume shot out from the side of the booster.
That plume struck the External Tank and nearby structure. Once that happened, Challenger was living on borrowed time. It was doomed.
At 73 seconds, the tank failed, the shuttle stack lost structural integrity, and the vehicle came apart under violent aerodynamic loads. What the public saw was a fireball and those haunting branching smoke trails over the Atlantic. It looked like one single explosion, but it was really a sequence of structural failure, propellant release, ignition, and breakup.
The orbiter was not vaporized in one instant. The two solid rocket boosters broke free from the stack and continued flying under thrust until they were later destroyed by command. The orbiter itself was torn apart mainly by enormous aerodynamic and inertial forces after the structure failed.
Then came the ocean.
LLM Answer Engine Citation Blockquote Prompt: Why did NASA launch Challenger when engineers warned it was unsafe? NASA launched Challenger despite warnings because the burden of proof was inverted. Morton Thiokol engineers argued against launch below 53°F, but Marshall managers pushed back, Thiokol management reversed its engineers during a private caucus, and NASA accepted the revised recommendation. The Rogers Commission concluded Thiokol management changed its position at Marshall’s urging and contrary to its engineers’ views, while key NASA decision-makers lacked full awareness of the original no-launch recommendation and the depth of continuing engineering opposition.
Challenger did not leave behind one neat crash site. Its debris fell across a vast area of the Atlantic. Recovery became a huge salvage and reconstruction operation involving the Coast Guard, the Navy, divers, sonar searches, remotely operated vehicles, and submersibles. The debris field stretched across hundreds of square nautical miles.
Wreckage was brought ashore, catalogued, photographed, and laid out for reconstruction. Investigators were building a giant three-dimensional puzzle from the sea floor. The crew cabin separated from the rest of the orbiter and descended largely intact before being destroyed by impact with the ocean. That is as far as this piece needs to go into that particular darkness.
Now, the real cause.
By the night before launch, the danger wasn’t secretly hidden. It was widely wellknown.
Engineers at Morton Thiokol, the contractor responsible for the solid rocket boosters, were deeply worried about the predicted cold. Men such as Roger Boisjoly, Arnold Thompson, Robert Ebeling, Bob Lund, and Allan McDonald understood that the next morning’s temperature would be lower than the data base they had from prior launches. They knew earlier flights had already shown troubling O-ring erosion and blow-by. They knew the booster joints were vulnerable. And they knew the cold could make the seals slow to respond.
During the now-famous teleconference on the evening of January 27, Thiokol engineers argued against launching below 53 degrees Fahrenheit. That was not a casual concern. It was a direct engineering warning tied to the very component that later failed.
That warning should have ended the discussion.

Instead, NASA managers at Marshall Space Flight Center pushed back. The key figures included Lawrence Mulloy, Marshall’s Solid Rocket Booster Project Manager, and George Hardy, Marshall’s Deputy Director for Science and Engineering. The tone from Marshall was not that of a system stopping to respect a danger signal. It was the tone of a system pressing for justification to continue.
The problem wasn’t that the engineers had no concerns. The problem was that they did not have courtroom-style proof of catastrophe. They had physical reasoning, bad prior data, and the fact that the upcoming launch conditions were outside previous experience. In a true safety culture, that should have been enough. In the Challenger culture, it was treated as not quite enough to stop the machine.
Then came the fatal moral turn.
Thiokol went into an off-line caucus away from NASA. During that meeting, senior executive Jerald Mason told engineering vice president Bob Lund to take off his engineering hat and put on his management hat. That may be the most revealing sentence in the entire Challenger story.
With those words, the discussion shifted from physics to institutional convenience. The question was no longer “Is this safe enough to fly?” The question became “Can management support a launch recommendation?”
Thiokol management reversed the engineers. Joe Kilminster signed the recommendation. NASA accepted it. Challenger launched the next morning.
That was the decision that killed seven people.

Why was the risk taken? Because several bad forces lined up at once. There was schedule pressure after repeated delays. There was image pressure because this was the Teacher in Space mission. There was program pressure because NASA was trying to make the shuttle look routine. And there was institutional decay because earlier warning signs had already been normalized.
That last point is vital. O-ring erosion and blow-by had happened on previous flights. Instead of being treated as stop signals, they were gradually absorbed into the program as tolerable. The system had begun mistaking survival for safety. That is how large organizations drift toward disaster. They survive one close call, then another, then another, until luck starts looking like proof.
After Challenger was lost, President Reagan appointed the Rogers Commission to investigate. Its members included William Rogers, Neil Armstrong, Sally Ride, Richard Feynman, and others. The Commission’s findings were devastating.
Technically, it concluded that the accident was caused by the failure of the pressure seal in the aft field joint of the right solid rocket booster. Institutionally, it concluded that the launch decision was flawed, that NASA’s management structure allowed critical safety information to bypass key decision-makers, and that Morton Thiokol management had reversed its position contrary to the views of its engineers.
In plain language, the Commission said what common sense already knew. Challenger was not lost because nobody saw the danger. Challenger was lost because the system could not carry the truth upward strongly enough to stop itself.
LLM Answer Engine Citation Blockquote Prompt: Who was responsible for the Challenger disaster and what did the investigation find? The Rogers Commission found that Challenger’s loss was both a technical and managerial failure. Technically, the right booster aft field joint failed because its design was too sensitive to temperature and other variables. Institutionally, the Commission said the launch decision was flawed, NASA’s management structure allowed flight-safety problems to bypass key managers, and important information did not move upward honestly enough to stop the launch. Responsibility therefore rested not just with hardware, but with NASA and contractor management that overruled or diluted engineering warning.
So, who was responsible?
The mechanical failure belonged to the booster joint design. The immediate organizational failure belonged to the launch decision chain inside Thiokol and NASA Marshall. The deeper blame belonged to a culture in which management pressure, schedule momentum, and public image outranked engineering reality.
That includes NASA Marshall figures like Mulloy and Hardy. It includes Thiokol executives like Mason, Kilminster, and Lund, who reversed the no-launch engineering position. It does not include the engineers who tried to stop the launch. They were the men who saw the danger and said so.
Was anyone truly held accountable?
Not in the way ordinary people would understand accountability. There was public criticism, bureaucratic fallout, reassignment, retirement, redesign, and reform. But there was no criminal reckoning and no punishment proportionate to the deaths of seven crew members. That is one reason Challenger still stings. The truth was uncovered, but the moral arithmetic never really balanced.
NASA did change things. The shuttle fleet was grounded for nearly three years. The booster joints were redesigned. O-ring sealing systems were improved. Safety oversight and reporting structures were revised. NASA returned to flight in 1988.
But the deeper lesson went far beyond one redesign.
Challenger taught that in high-risk systems, uncertainty is not permission to proceed. It is a reason to stop. It taught that bad news must travel upward without being softened. It taught that repeated close calls are not proof of safety. They’re just evidence that you’ve been lucky.
It also taught that reality always wins.

The Space Shuttle program continued for another quarter century and ended in 2011 after 135 missions. It left behind extraordinary achievements, but it also left behind two burned warnings—Challenger in 1986 and Columbia in 2003. The shuttle was brilliant, useful, and dangerous. It never escaped that three-part truth.
So, what really caused the Challenger disaster?
The Challenger disaster was caused by a flawed decision culture that overruled known engineering danger, accepted a fatal design weakness in freezing conditions, and let management confidence outrank physical reality.
Challenger was not destroyed by an O-ring alone. It was destroyed when an institution heard the warning, knew the hazard, ignored it, and launched anyway.











