“Medical examiner responds to second sleep-related infant death this week.”
 This headline got my attention when it was posted online Nov 13, 2014, by Shakara Robinson of WDJT58 in Milwaukee. I’ve been meaning to write about Sudden Infant Death Syndrome, or SIDS, since I started DyingWords as I feel it’s the most tragic, misunderstood, and preventable type of death.
This headline got my attention when it was posted online Nov 13, 2014, by Shakara Robinson of WDJT58 in Milwaukee. I’ve been meaning to write about Sudden Infant Death Syndrome, or SIDS, since I started DyingWords as I feel it’s the most tragic, misunderstood, and preventable type of death.
The article continued…
The Milwaukee County Medical Examiner’s Office responded to the death of a one-month-old infant Wednesday morning near 27th and Meinecke. Officials say the baby boy was pronounced dead at the home in the 2400 block of N. 27th Street just after 8 a.m. Initial reports suggest the baby was sleeping with his mother. An autopsy is scheduled for Friday. This is the second sleep-related infant death the Milwaukee County Medical Examiner’s Office has reported this week. A 10-day-old baby boy was pronounced dead November 10 near 81st and Oklahoma after sleeping in bed with his mother and a sibling.
I’ve attended too many SIDS cases in my time as a police officer and coroner. They are, by far, the most difficult deaths to investigate – not because of the lack of medical evidence – it’s the emotional trauma suffered by the families which sticks to the investigators.
 Sudden Infant Death Syndrome is the unexplained and unexpected death of a seemingly healthy baby aged less than 1 year old. These deaths are legally classified as SIDS if the cause can’t be explained after a thorough investigation that includes an autopsy, examination of the death scene, and review of the clinical history.
Sudden Infant Death Syndrome is the unexplained and unexpected death of a seemingly healthy baby aged less than 1 year old. These deaths are legally classified as SIDS if the cause can’t be explained after a thorough investigation that includes an autopsy, examination of the death scene, and review of the clinical history.
SIDS is sometimes termed ‘SUID’ for Sudden Unexplained Infant Death. Historically it’s been called crib death because many infants die in their cribs. It’s been occurring as long as humanity has been around.
SIDS is also different from positional asphyxia, accidental smothering, and accidental strangulation which are provable causes of death. In SIDS, the infant just stops breathing without an external event.
SIDS is the third leading cause of infant mortality in the world (following malnutrition and infectious disease) and it’s the leading cause of death among infants aged 1– 4 months. Although the overall rate of SIDS has declined by more than 50% since 1990, rates for black and aboriginal infants remain disproportionately higher than the rest of the population. Curiously, it occurs frequently in colder months and in homes with many occupants.
There’s no proven death mechanism for SIDS, yet it’s a recognized cause of death (COD). It appears that SIDS is associated with abnormalities in the portion of an infant’s brain that controls breathing and arousal from sleep.
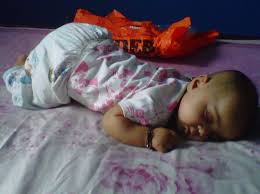 Infants are at their highest risk for SIDS during sleep. Typically, the infant is found dead after having been put to bed and there’s no sign of struggle or abuse. For some reason they just stopped breathing which, in turn, causes hypoxia or a lack of oxygenated blood to the brain resulting in cardiac arrest.
Infants are at their highest risk for SIDS during sleep. Typically, the infant is found dead after having been put to bed and there’s no sign of struggle or abuse. For some reason they just stopped breathing which, in turn, causes hypoxia or a lack of oxygenated blood to the brain resulting in cardiac arrest.
Most SIDS cases occur when babies are placed on their stomachs to sleep rather than on their backs or sides. Some researchers have hypothesized that stomach sleeping puts pressure on a child’s jaw, therefore narrowing the airway and hampering breathing.
Another theory is that stomach sleeping increases an infant’s risk of “rebreathing” his or her own exhaled air, particularly if the infant is sleeping on a soft mattress or with bedding, stuffed toys, or a pillow near the face. In that scenario, the soft surface creates a small enclosure around the baby’s mouth and traps exhaled air. As the baby breathes exhaled air, the oxygen level in the body drops and carbon dioxide accumulates. Eventually, this lack of oxygen contributes to SIDS.
Also, infants who succumb to SIDS may have an abnormality in the arcuate nucleus, a part of the brain that controls breathing during sleep. If a baby breathes stale air and doesn’t get enough oxygen, the brain triggers the baby to wake up and cry. That movement changes the breathing and heart rate, making up for the lack of oxygen. But a problem with the arcuate nucleus deprives the baby of this involuntary reaction.
Many doctors believe multiple factors contribute to SIDS.
 Sleeping on stomachs
Sleeping on stomachs- Exposure to tobacco smoke in the womb or after birth
- Sleeping in bed with parents
- Premature birth
- Being a twin or triplet
- Born to a teen mother
Regardless, the biggest preventive of SIDS is always placing your little one on the back to sleep.
These tips from the Centers for Disease Control address the risk of succumbing to SIDS:
- Place her on a firm mattress to sleep, never on a pillow, waterbed, sheepskin, couch, chair, or other soft surface. To prevent rebreathing, do not put blankets, comforters, stuffed toys, or pillows nearby.
- Don’t use bumper pads in cribs. Bumper pads can suffocate or strangulate.
- Make sure he’s immunized. Babies who are immunized have a 50% lower risk of SIDS.
- Make sure she’s not too warm while sleeping. Keep the room at a temperature that feels comfortable for an adult in a short-sleeve shirt. Some researchers suggest babies who get too warm go into a deeper sleep, making more difficult to awaken.
- Do not smoke, drink, or use drugs while pregnant and do not expose your baby to secondhand smoke. Infants of smoking mothers during pregnancy are 3 times more likely to die of SIDS than smoke-free moms. Exposure to secondhand smoke doubles your baby’s risk of SIDS. Researchers speculate that smoking affects the central nervous system, starting prenatally, and continuing after birth, which places your baby at increased risk.
- Receive early and regular prenatal care.
- Make sure he has regular checkups.
- Breastfeed, if possible. There’s evidence that breastfeeding decreases the incidence of SIDS. Breast milk naturally immunizes her from infections that increase the risk of SIDS.
- If he has Gastroesophangael Reflux Disease (GERD), be sure to follow your doctor’s guidelines on feeding and sleep positions.
- Put her to sleep with a pacifier during the first year of life. If she rejects the pacifier, don’t force it. Pacifiers are linked with lower risk of SIDS. If you’re breastfeeding, try to wait until after she’s 1 month old so that breastfeeding can be established.
- While he can be brought into your bed for nursing or comforting, put him back in his crib or bassinet when you’re ready to sleep. It’s okay to keep him in your room. Just don’t run the risk of rolling over and smothering him.
- Don’t assume others will place her to sleep in the correct position. Insist on it. Advise sitters and child care personnel not to use the stomach position to calm an upset baby.
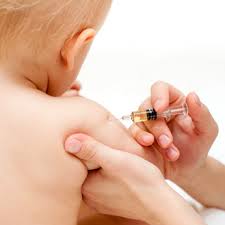 Vaccinations have been a suspect in the cause of SIDS. From 2 – 4 months old, babies begin getting primary vaccinations. Co-incidentally, this is the peak age for SIDS. The timing of these two events might seem suspicious, however exhaustive studies conclude vaccinations are not a SIDS risk factor. Inversely, vaccinations are the leading cause of infant survival.
Vaccinations have been a suspect in the cause of SIDS. From 2 – 4 months old, babies begin getting primary vaccinations. Co-incidentally, this is the peak age for SIDS. The timing of these two events might seem suspicious, however exhaustive studies conclude vaccinations are not a SIDS risk factor. Inversely, vaccinations are the leading cause of infant survival.
Now, I have a personal suspect in infant deaths that are mistakenly classified as SIDS.
 This culprit is Stachybotrys chartarum. It’s an extremely toxic black mold found in cellulose rich building materials which requires high heat and moisture in order to grow and is associated with wet gypsum material and wallpaper.
This culprit is Stachybotrys chartarum. It’s an extremely toxic black mold found in cellulose rich building materials which requires high heat and moisture in order to grow and is associated with wet gypsum material and wallpaper.
Health problems related to this nasty mold have been documented in humans and animals since the 1930s. It’s also considered a likely candidate for the Biblical condition mistranslated as “leprosy”.
Today, Stachybotrys is linked to sick building syndrome. It’s not firmly established in scientific literature, but I find it very suspicious that the disproportionately high rate of SIDS in blacks and aboriginals can be linked to environmental conditions where Stachybotrys is prominent.
I’m not being racist here. I’m being a realist. The majority of SIDS deaths I attended were in the Canadian aboriginal (First Nations) demographic. Looking back at my notes, these deaths were mostly in the cool seasons when the residential heat was artificially high and the ventilation was low. The social state of these communities leads to a high occupancy ratio and an extremely high humidity factor in their houses – the perfect breeding ground for toxic black mold.
 My theory continues. The most vulnerable climate-exposure period for infants is when they’re building their immune system – 1 to 4 months. Contacting an environmental airborne pathogen like Stachybotrys can result in a mycotoxicosis causing a metabolic, respiratory, or cardiac disorder which could trigger sudden death.
My theory continues. The most vulnerable climate-exposure period for infants is when they’re building their immune system – 1 to 4 months. Contacting an environmental airborne pathogen like Stachybotrys can result in a mycotoxicosis causing a metabolic, respiratory, or cardiac disorder which could trigger sudden death.
I’m not saying most SIDS cases are pathogen related. Ultimately, all deaths have an anatomical cause that unplugs the central nervous system. I just think that many infant deaths written off as SIDS have a root cause hidden in their environment.

I’ve heard that SIDS is a diagnosis of exclusion rather than inclusion. There’s a case right now on HLN where they didn’t check on the baby for 16 hrs and are now facing the wrath of the internet as well as the denigration of the police.
For this situation, personally I think it’s wrong they are so hard on the parents. Hard day’s work, you come home, you & hubby get buzzed thinking baby is sleeping. You go to bed thinking hubby will check on her before he comes, he thinks you checked on her before you lay down. Can you imagine what they suffered finding their baby dead? I’m 57, but when I was young I got a buzz on with friends when my kids were in bed for the night a couple or few times. I always checked them before I went to bed, They were ok. Why would these parents expect it to be any different if the missed 1 check??